 Based on cell surface expression markers and specialized function, T cells are divided into the classic dichotomy of CD4 + and CD8 + T cells. T cells are a central component of protective immunity to severe pneumonia ( Chen and Kolls, 2013). Optimal therapies for severe pneumonia must address both pathogen and host, and a comprehensive characterization of the innate and adaptive immune response during severe pneumonia is a critical step toward achieving that goal. Thus, leveraging non-traditional strategies focusing on host-derived immune mechanisms that promote restoration of tissue architecture and physiological function are critical for improved patient outcomes and survival ( Theuretzbacher and Piddock, 2019). Furthermore, even after receiving optimal antimicrobial therapy, mortality remains exceedingly high for patients with Gram-negative pneumonia ( Feng et al., 2019). 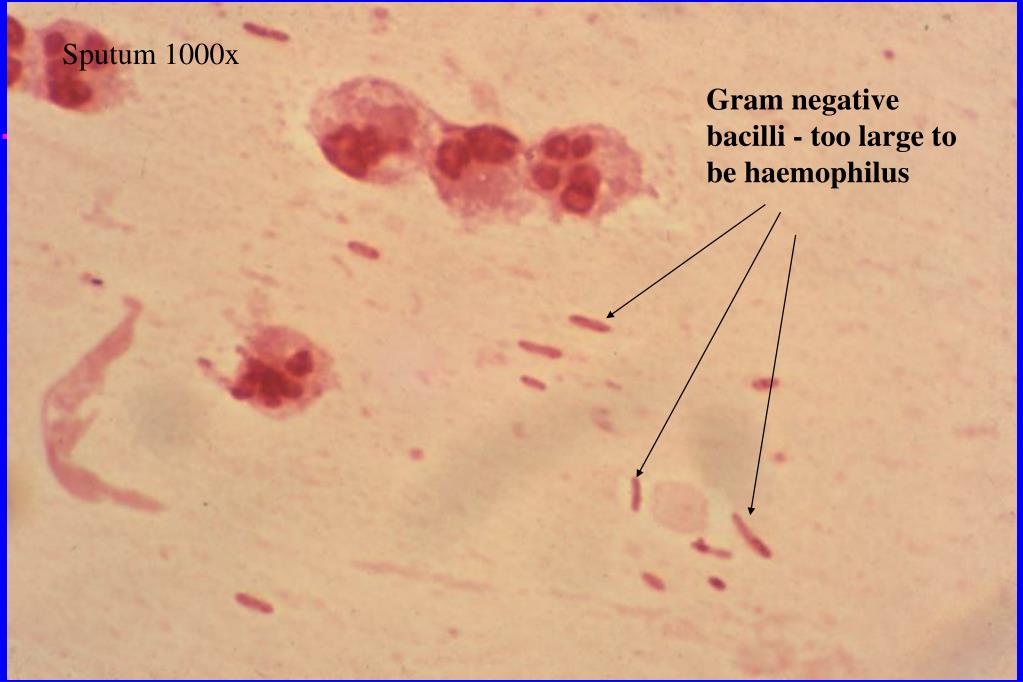
Successful resolution of any severe infectious disease requires a multipronged approach to management, but work in severe pneumonia has primarily focused on developing therapeutics that target specific pathogens. Four of these six hypervirulent pathogens are Gram-negative bacteria, underscoring the critical need to address gaps in the treatment of lower respiratory tract infection from these pathogens. A cohort of nosocomial pathogens with significant multi-drug resistant (MDR) and extensively drug resistant (XDR) characteristics are grouped together with the acronym, ESKAPE ( Enterococcus faecium, Staphylococcus aureus, Klebsiella pneumoniae, Acinetobacter baumannii, Pseudomonas aeruginosa, and Enterobacter spp), due to their ability to ‘escape’ traditional antimicrobial therapy ( Mulani et al., 2019). Despite advances in diagnosis and management of severe pneumonia, it remains associated with high rates of mortality, prolonged hospitalizations and substantial healthcare expenditures ( Torres et al., 2021). Gram-negative bacteria are a leading cause of severe hospital-acquired pneumonia/ventilator-associated pneumonia (HAP/VAP), which can progress to acute respiratory distress syndrome (ARDS), multi-organ failure, and death ( Jean et al., 2020). We highlight key factors in these responses that have potential for therapeutic targeting, as well as the gaps in current knowledge to be focused on in future work. In this review, we focus on the adaptive T cell responses to pneumonia induced by Klebsiella pneumoniae, Pseudomonas aeruginosa, and Acinetobacter baumannii. Adaptive immunity plays a pivotal role in modulating these processes, thus affecting the incidence and severity of pneumonia. Hence, an alternative approach is to focus on the disease tolerance components that mediate immune resistance and enhance tissue resilience. 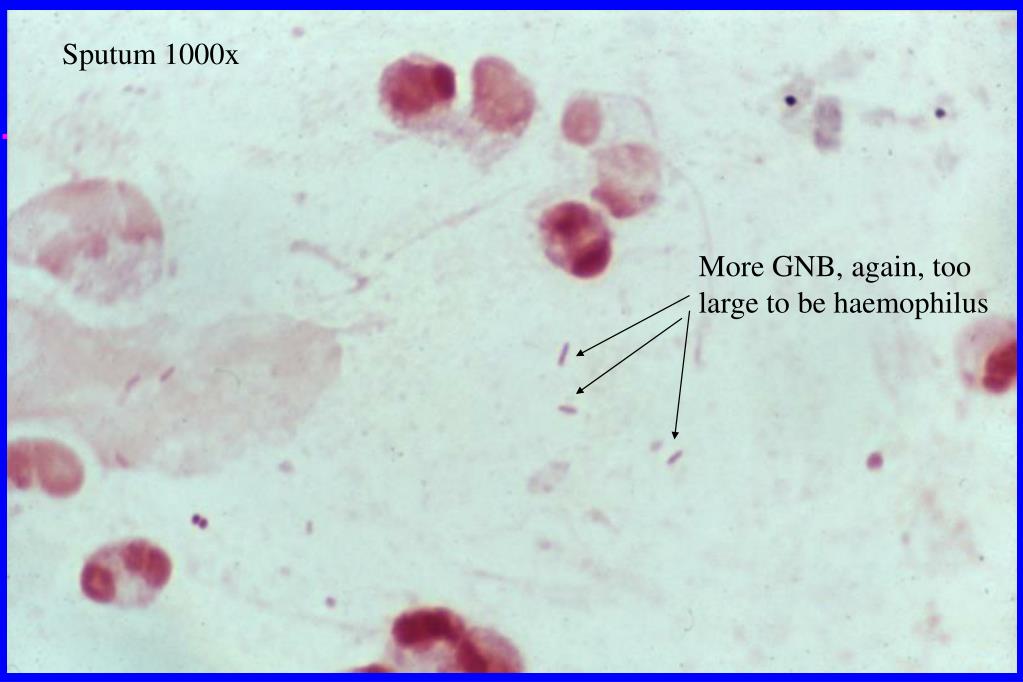 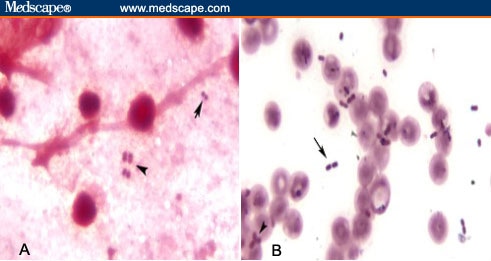
Despite advances in diagnosis and treatment, the rise of multidrug-resistant organisms and hypervirulent strains demonstrates that there will continue to be challenges with traditional treatment strategies using antibiotics. Pneumonia is one of the leading causes of morbidity and mortality worldwide and Gram-negative bacteria are a major cause of severe pneumonia.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
